A Predictive Model for Lateral Cervical Lymph Node Metastasis in Thyroid Cancer
DOI:
https://doi.org/10.71321/5r3ppj45Keywords:
Papillary thyroid carcinoma, Lateral lymph node metastasis, Machine learning, Clinical prediction model, SHapley Additive exPlanations (SHAP)Abstract
Objective: To investigate the predictive factors for lateral lymph node metastasis (LLNM) in patients with papillary thyroid carcinoma (PTC) and to develop an individualized prediction model.
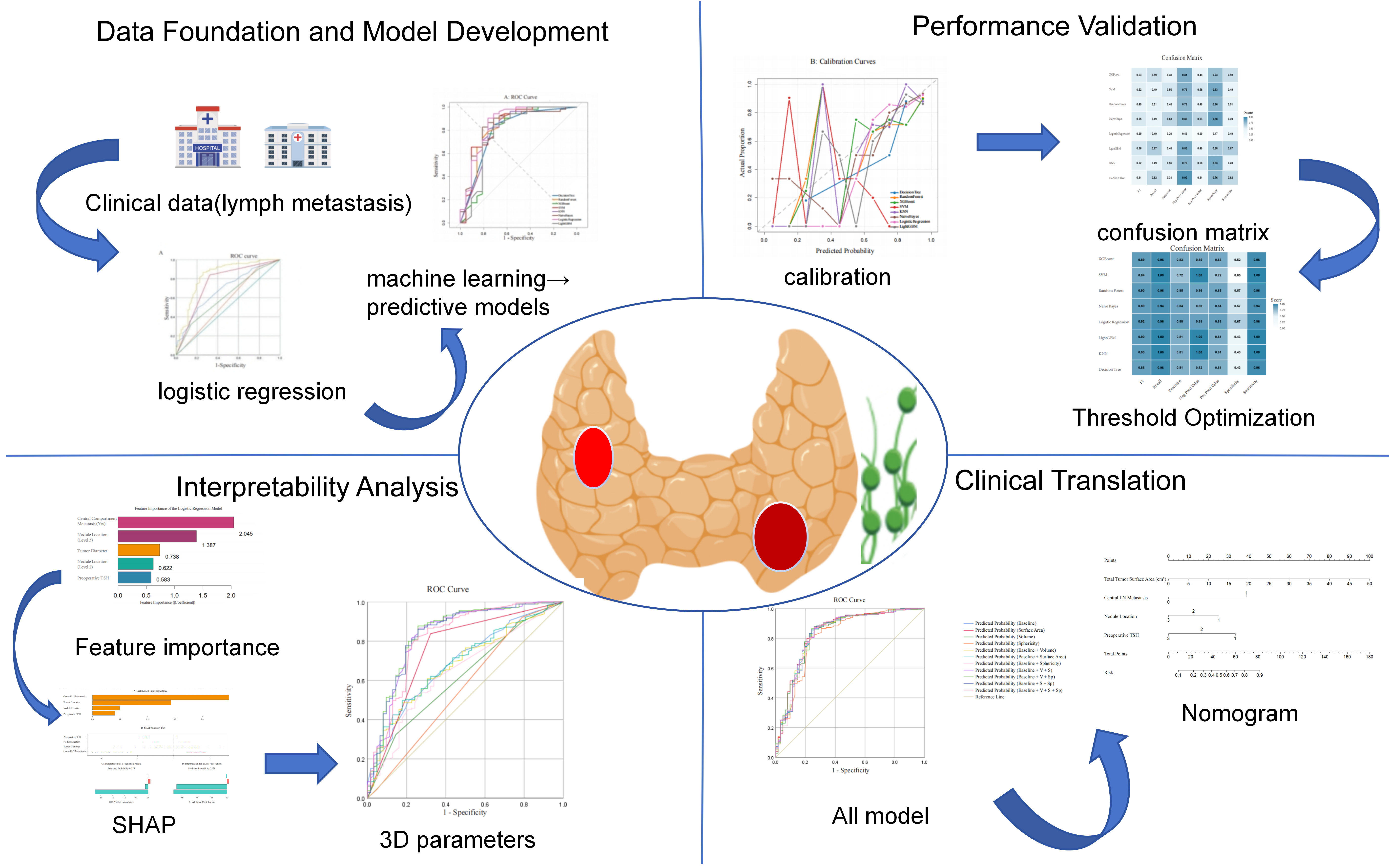
Methods: Clinical data from 241 PTC patients who underwent lateral neck dissection were analyzed. Logistic regression and machine learning methods were employed to identify predictive factors and construct a model. The predictive value of three-dimensional morphological parameters (total tumor surface area and total tumor volume) was also evaluated.
Results: Maximum tumor diameter, central lymph node metastasis, preoperative Thyroid-Stimulating Hormone (TSH), and tumor location were identified as independent predictors of LLNM. A baseline combined model based on maximum tumor diameter showed good predictive performance (AUC 0.832). Furthermore, three-dimensional parameters (total surface area and total volume) demonstrated complementary predictive potential compared to the baseline model.
Conclusion: An effective clinical prediction model for assessing LLNM risk was successfully developed. Three-dimensional morphological parameters represent promising predictive indicators with potential complementary value.
References
[1] Miranda-Filho A, Lortet-Tieulent J, Bray F, Cao B, Franceschi S, Vaccarella S, et al. Thyroid cancer incidence trends by histology in 25 countries: a population-based study. Lancet Diabetes Endocrinol. 2021;9:225–34. https://doi.org/10.1016/S2213-8587(21)00027-9.
[2] Bray F, Laversanne M, Sung H, Ferlay J, Siegel RL, Soerjomataram I, et al. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2024;74:229–63. https://doi.org/10.3322/caac.21834.
[3] Haugen BR, Alexander EK, Bible KC, Doherty GM, Mandel SJ, Nikiforov YE, et al. 2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer. Thyroid Off J Am Thyroid Assoc. 2016;26:1–133. https://doi.org/10.1089/thy.2015.0020.
[4] Siegel RL, Miller KD, Wagle NS, Jemal A. Cancer statistics, 2023. CA Cancer J Clin. 2023;73:17–48. https://doi.org/10.3322/caac.21763.
[5] Zaydfudim V, Feurer ID, Griffin MR, Phay JE. The impact of lymph node involvement on survival in patients with papillary and follicular thyroid carcinoma. Surgery. 2008;144:1070–7; discussion 1077-1078. https://doi.org/10.1016/j.surg.2008.08.034.
[6] Basolo F, Macerola E, Poma AM, Torregrossa L. The 5th edition of WHO classification of tumors of endocrine organs: changes in the diagnosis of follicular-derived thyroid carcinoma. Endocrine. 2023;80:470–6. https://doi.org/10.1007/s12020-023-03336-4.
[7] Shen G, Ma H, Huang R, Kuang A. Predicting large-volume lymph node metastasis in the clinically node-negative papillary thyroid microcarcinoma: a retrospective study. Nucl Med Commun. 2020;41:5–10. https://doi.org/10.1097/MNM.0000000000001119.
[8] Smith VA, Sessions RB, Lentsch EJ. Cervical lymph node metastasis and papillary thyroid carcinoma: does the compartment involved affect survival? Experience from the SEER database. J Surg Oncol. 2012;106:357–62. https://doi.org/10.1002/jso.23090.
[9] de Meer SGA, Dauwan M, de Keizer B, Valk GD, Borel Rinkes IHM, Vriens MR. Not the number but the location of lymph nodes matters for recurrence rate and disease-free survival in patients with differentiated thyroid cancer. World J Surg. 2012;36:1262–7. https://doi.org/10.1007/s00268-012-1427-1.
[10] Ruan J, Chen Z, Chen S, Xu Z, Wen L, Mao Z, et al. Lateral lymph node metastasis in papillary thyroid microcarcinoma: a study of 5241 follow-up patients. Endocrine. 2024;83:414–21. https://doi.org/10.1007/s12020-023-03486-5.
[11] Haddad RI, Bischoff L, Ball D, Bernet V, Blomain E, Busaidy NL, et al. Thyroid Carcinoma, Version 2.2022, NCCN Clinical Practice Guidelines in Oncology. J Natl Compr Cancer Netw JNCCN. 2022;20:925–51. https://doi.org/10.6004/jnccn.2022.0040.
[12] Fei Y, Wang B, Yao X, Wu J. Factors associated with occult lateral lymph node metastases in patients with clinically lymph node negative papillary thyroid carcinoma: a systematic review and meta-analysis. Front Endocrinol. 2024;15:1353923. https://doi.org/10.3389/fendo.2024.1353923.
[13] Zhang S, Liu R, Wang Y, Zhang Y, Li M, Wang Y, et al. Ultrasound-Base Radiomics for Discerning Lymph Node Metastasis in Thyroid Cancer: A Systematic Review and Meta-analysis. Acad Radiol. 2024;31:3118–30. https://doi.org/10.1016/j.acra.2024.03.012.
[14] Mulla MG, Knoefel WT, Gilbert J, McGregor A, Schulte K-M. Lateral cervical lymph node metastases in papillary thyroid cancer: a systematic review of imaging-guided and prophylactic removal of the lateral compartment. Clin Endocrinol (Oxf). 2012;77:126–31. https://doi.org/10.1111/j.1365-2265.2012.04336.x.
[15] Alabousi M, Alabousi A, Adham S, Pozdnyakov A, Ramadan S, Chaudhari H, et al. Diagnostic Test Accuracy of Ultrasonography vs Computed Tomography for Papillary Thyroid Cancer Cervical Lymph Node Metastasis: A Systematic Review and Meta-analysis. JAMA Otolaryngol-- Head Neck Surg. 2022;148:107–18. https://doi.org/10.1001/jamaoto.2021.3387.
[16] Zhang Y, Lu Y-Y, Li W, Zhao J-H, Zhang Y, He H-Y, et al. Lymphatic Contrast-enhanced US to Improve the Diagnosis of Cervical Lymph Node Metastasis from Thyroid Cancer. Radiology. 2023;307:e221265. https://doi.org/10.1148/radiol.221265.
[17] Lin S, Zhong Y, Lin Y, Liu G. Prediction model for lateral lymph node metastasis of papillary thyroid carcinoma in children and adolescents based on ultrasound imaging and clinical features: a retrospective study. BMC Med Imaging. 2024;24:228. https://doi.org/10.1186/s12880-024-01384-4.
[18] Yang Z, Wang X, Tao T, Zou J, Qiu Z, Wang L, et al. Diagnostic value of contrast-enhanced ultrasonography in the preoperative evaluation of lymph node metastasis in papillary thyroid carcinoma: a single-center retrospective study. BMC Surg. 2023;23:325. https://doi.org/10.1186/s12893-023-02199-w.
[19] Tee YY, Lowe AJ, Brand CA, Judson RT. Fine-needle aspiration may miss a third of all malignancy in palpable thyroid nodules: a comprehensive literature review. Ann Surg. 2007;246:714–20. https://doi.org/10.1097/SLA.0b013e3180f61adc.
[20] Shao L, Wang Z, Dong W, Sun W, Zhang H. Risk factors associated with preferential lateral lymph node metastasis in papillary thyroid carcinoma. Cancer Med. 2023;12:20670–6. https://doi.org/10.1002/cam4.6567.
[21] So YK, Kim M-J, Kim S, Son Y-I. Lateral lymph node metastasis in papillary thyroid carcinoma: A systematic review and meta-analysis for prevalence, risk factors, and location. Int J Surg Lond Engl. 2018;50:94–103. https://doi.org/10.1016/j.ijsu.2017.12.029.
[22] Zhao L, Wu F, Zhou T, Lu K, Jiang K, Zhang Y, et al. Risk factors of skip lateral cervical lymph node metastasis in papillary thyroid carcinoma: a systematic review and meta-analysis. Endocrine. 2022;75:351–9. https://doi.org/10.1007/s12020-021-02967-9.
[23] Zhao H, Huang T, Li H. Risk factors for skip metastasis and lateral lymph node metastasis of papillary thyroid cancer. Surgery. 2019;166:55–60. https://doi.org/10.1016/j.surg.2019.01.025.
[24] Mizuno K, Takeuchi M, Kanazawa Y, Kitamura M, Ide K, Omori K, et al. Recurrent laryngeal nerve paralysis after thyroid cancer surgery and intraoperative nerve monitoring. The Laryngoscope. 2019;129:1954–60. https://doi.org/10.1002/lary.27698.
[25] Yazıcıoğlu MÖ, Yılmaz A, Kocaöz S, Özçağlayan R, Parlak Ö. Risks and prediction of postoperative hypoparathyroidism due to thyroid surgery. Sci Rep. 2021;11:11876. https://doi.org/10.1038/s41598-021-91277-1.
[26] Hassan I, Hassan L, Bacha F, Alsalameh M, Qatee O, Hassan W. Clinico-pathological initial outcome of a newly adopted novel surgical technique for nodal metastatic thyroid cancer at a large-volume centre in a high-income developing country. Front Surg. 2023;10:1204230. https://doi.org/10.3389/fsurg.2023.1204230.
[27] Zhang X, Chen W, Fang Q, Fan J, Feng L, Guo L, et al. Lateral Lymph Node Metastases in T1a Papillary Thyroid Carcinoma: Stratification by Tumor Location and Size. Front Endocrinol. 2021;12:716082. https://doi.org/10.3389/fendo.2021.716082.
[28] Bae SY, Jung SP, Choe J-H, Kim JS, Kim JH. Prediction of lateral neck lymph node metastasis according to preoperative calcitonin level and tumor size for medullary thyroid carcinoma. Kaohsiung J Med Sci. 2019;35:772–7. https://doi.org/10.1002/kjm2.12122.
[29] Yu Q, Hao W, He Y, Ruan X, Liu L, Yun X, et al. Multi-omics analysis unveils dysregulation of the tumor immune microenvironment and development of a machine learning-based multi-gene classifier for predicting lateral lymph node metastasis in papillary thyroid carcinoma. Endocrine. 2025;90:172–87. https://doi.org/10.1007/s12020-025-04308-6.
[30] Ywata de Carvalho A, Kohler HF, Gomes CC, Vartanian JG, Kowalski LP. Predictive factors for recurrence of papillary thyroid carcinoma: analysis of 4,085 patients. Acta Otorhinolaryngol Ital Organo Uff Della Soc Ital Otorinolaringol E Chir Cerv-facc. 2021;41:236–42. https://doi.org/10.14639/0392-100X-N1412.
[31] Wada N, Duh Q-Y, Sugino K, Iwasaki H, Kameyama K, Mimura T, et al. Lymph Node Metastasis From 259 Papillary Thyroid Microcarcinomas. Ann Surg. 2003;237:399–407. https://doi.org/10.1097/01.SLA.0000055273.58908.19.
[32] Zhan S, Luo D, Ge W, Zhang B, Wang T. Clinicopathological predictors of occult lateral neck lymph node metastasis in papillary thyroid cancer: A meta-analysis. Head Neck. 2019;41:2441–9. https://doi.org/10.1002/hed.25762.
[33] Hu D, Lin H, Zeng X, Wang T, Deng J, Su X. Risk Factors for and Prediction Model of Skip Metastasis to Lateral Lymph Nodes in Papillary Thyroid Carcinoma. World J Surg. 2020;44:1498–505. https://doi.org/10.1007/s00268-019-05332-0.
[34] Feng J-W, Qin A-C, Ye J, Pan H, Jiang Y, Qu Z. Predictive Factors for Lateral Lymph Node Metastasis and Skip Metastasis in Papillary Thyroid Carcinoma. Endocr Pathol. 2020;31:67–76. https://doi.org/10.1007/s12022-019-09599-w.
[35] Wu X, Li B, Zheng C, He X. Risk factors for skip metastasis in patients with papillary thyroid microcarcinoma. Cancer Med. 2023;12:7560–6. https://doi.org/10.1002/cam4.5507.
[36] Qubain SW, Nakano S, Baba M, Takao S, Aikou T. Distribution of lymph node micrometastasis in pN0 well-differentiated thyroid carcinoma. Surgery. 2002;131:249–56. https://doi.org/10.1067/msy.2002.120657.
[37] Back K, Kim JS, Kim J-H, Choe J-H. Superior Located Papillary Thyroid Microcarcinoma is a Risk Factor for Lateral Lymph Node Metastasis. Ann Surg Oncol. 2019;26:3992–4001. https://doi.org/10.1245/s10434-019-07587-2.
[38] Yu Y, Ouyang W, Huang Y, Huang H, Wang Z, Jia X, et al. Artificial intelligence-based multi-modal multi-tasks analysis reveals tumor molecular heterogeneity, predicts preoperative lymph node metastasis and prognosis in papillary thyroid carcinoma: a retrospective study. Int J Surg Lond Engl. 2025;111:839–56. https://doi.org/10.1097/JS9.0000000000001875.
[39] Yu S, Liu C, Hou Y, Li J, Guo Z, Chen X, et al. Integrative metabolomic characterization identifies plasma metabolomic signature in the diagnosis of papillary thyroid cancer. Oncogene. 2022;41:2422–30. https://doi.org/10.1038/s41388-022-02254-5.
[40] Zhang L, Zhang J, Fan S, Zhong Y, Li J, Zhao Y, et al. A case-control study of urinary concentrations of bisphenol A, bisphenol F, and bisphenol S and the risk of papillary thyroid cancer. Chemosphere. 2023;312 Pt 1:137162. https://doi.org/10.1016/j.chemosphere.2022.137162.
Type
Published
Issue
Section
License
Copyright (c) 2026 Head and Neck Diseases Conflux

This work is licensed under a Creative Commons Attribution 4.0 International License.







