Developmental Outcomes Following Early Cochlear Implantation in Infants and Toddlers: a Comparative Study with Normal-hearing Peers
DOI:
https://doi.org/10.71321/prwgkz02Keywords:
Cochlear implants, Development, Auditory, SpeechAbstract
Objective: To evaluate whether early cochlear implant (CI) use can significantly and positively change hearing and speech abilities during a child’s development.
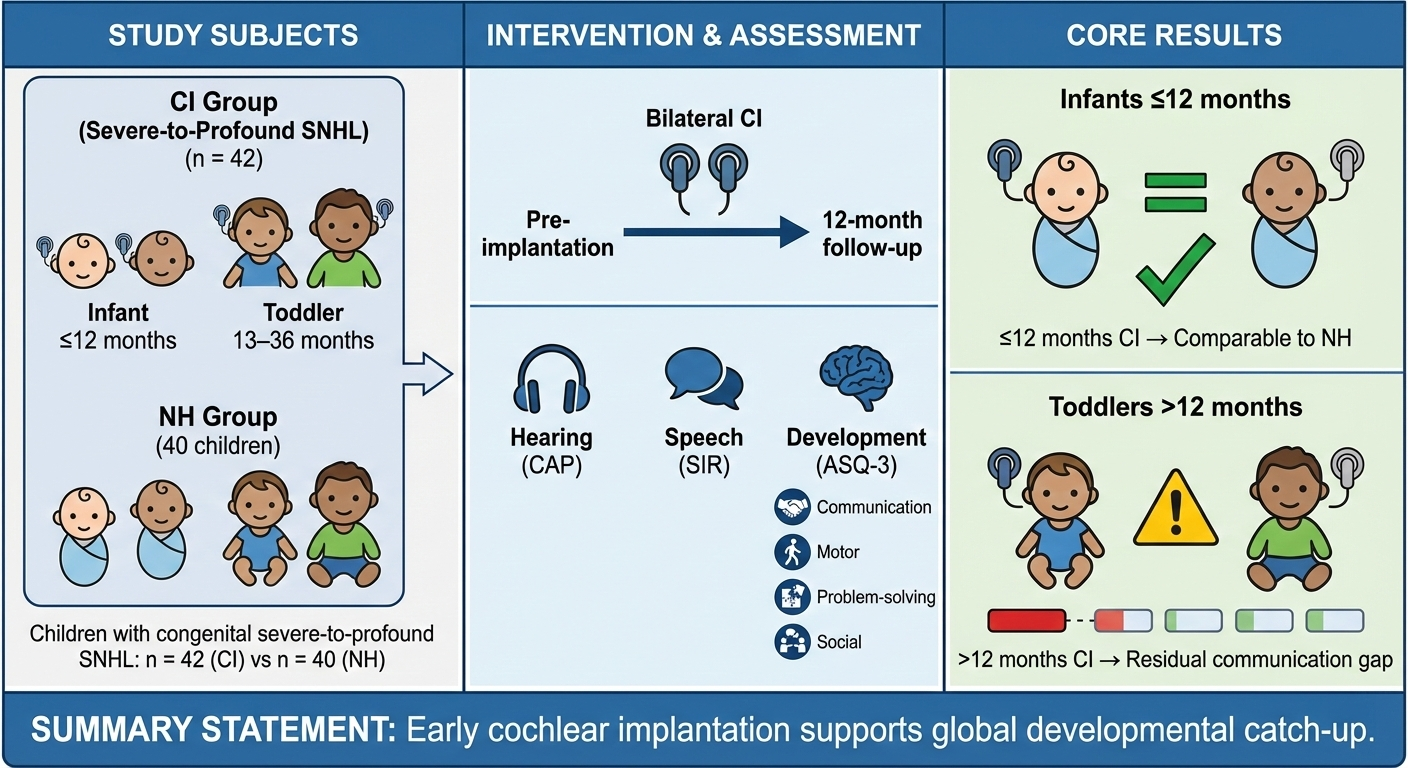
Methods: The present study included 42 children with bilateral CIs (8–36 months) and 40 age-matched children with normal hearing (NH) (6–48 months). Ages & Stages Questionnaires, Third Edition (ASQ-3); Categories of Auditory Performance (CAP); Speech Intelligibility Rate (SIR) were used.
Results: Twelve months after receiving bilateral CIs, the hearing status of the infants (1–12 months) and toddlers (13–36 months) had improved significantly. Infants using CIs were comparable to those with NH in all ASQ-3 aspects (p > 0.05). For toddlers, there was a post-implantation improvement in the gross motor, problem solving, and personal social domains (p > 0.05). However, there were still gaps in the communication domain (p < 0.001). Multivariate analysis revealed that pre-implantation hearing aid usage duration, schooling, SIR score, communication, and caregiver education level significantly influenced post implantation outcomes.
Conclusions: With CI use, infants and toddlers with congenital sensorineural hearing loss showed improvements in auditory perception, speech production, and developmental abilities. Infant implant recipients performed better in all areas of development than toddlers, comparable to with NH children. Hearing aid use, language rehabilitation training, caregivers’ education level, and communication method were all highly correlated with the overall development of the children.
References
[1] Li FF, Wang JP, Zhang WJ, Zhou PT, Fan M, Cai NN, et al. (2025). Trends and mechanisms of Alzheimer's disease and hearing impairment: A 20-year perspective. Ageing Res Rev, 110, 102799. https://doi.org/10.1016/j.arr.2025.102799
[2] Li FF, Fu ZY, Han K, Liang BY, Han YX, Liu YH, et al. (2025). Trends and driving factors of age-related hearing loss and severity over 30 years: a cross-sectional study. BMC Geriatr, 25(1), 387. https://doi.org/10.1186/s12877-025-06066-6
[3] Jiang CY, Han K, Yang F, Yin SY, Yin SY, Zhang L, et al. (2023). Global, regional, and national prevalence of hearing loss from 1990 to 2019: A trend and health inequality analyses based on the Global Burden of Disease Study 2019. Ageing Res Rev, 92, 102124. https://doi.org/10.1016/j.arr.2023.102124
[4] NIH Consensus Conference. (1995). Cochlear implants in adults and children. JAMA, 274(24), 1955–1961. https://doi.org/10.1001/jama.1995.03530240061037
[5] Incerti PV, Ching TYC, Hou S, Van Buynder P, Flynn C, & Cowan R. (2018). Programming characteristics of cochlear implants in children: effects of etiology and age at implantation. Int J Audiol, 57(sup2), S27-S40. https://doi.org/10.1080/14992027.2017.1370139
[6] Dettman SJ, Dowell RC, Choo D, Arnott W, Abrahams Y, Davis A, et al. (2016). Long-term communication outcomes for children receiving cochlear implants younger than 12 months: a multicenter study. Otol Neurotol, 37, e82–e95. https://doi.org/10.1097/MAO.0000000000000915
[7] Holman MA, Carlson ML, Driscoll CL, Beatles SP, Peterson AM, Sladen DP, et al. (2013). Cochlear implantation in children 12 months of age and younger. Otol Neurotol, 34, 251–258. https://doi.org/10.1097/mao.0b013e31827d0922
[8] Dorman MF, Sharma A, Gilley P, Martin K, & Roland P. (2007). Central auditory development: evidence from CAEP measurements in children fit with cochlear implants. J Commun Disord, 40, 284–294. https://doi.org/10.1016/j.jcomdis.2007.03.007
[9] Sharma A, Gilley PM, Dorman MF, & Baldwin R. (2007). Deprivation-induced cortical reorganization in children with cochlear implants. Int J Audiol, 46, 494–499. https://doi.org/10.1080/14992020701524836
[10] Sharma A, Campbell J, & Cardon G. (2009). Cortical development, plasticity and re-organization in children with cochlear implants. J Commun Disord, 42, 272–279. https://doi.org/10.1016/j.jcomdis.2009.03.003
[11] Niparko JK, Hoffman M, Tiddens E, & Quittner AL. (2018). Comparisons of visual attention in school-age children with cochlear implants versus hearing peers and normative data. Hear Res, 359, 91–100. https://doi.org/10.1016/j.heares.2018.01.002
[12] Lund E, & Dinsmoor J. (2016). Taxonomic knowledge of children with and without cochlear implants. Lang Speech Hear Serv Sch, 47, 236–245. https://doi.org/10.1044/2016_LSHSS-15-0032
[13] Harris MS, Kronenberger WG, Gao S, Hoen HM, Miyamoto RT, & Pisoni DB. (2013). Verbal short-term memory development and spoken language outcomes in deaf children with cochlear implants. Ear Hear, 34, 179–192. https://doi.org/10.1097/AUD.0b013e318269ce50
[14] Boons T, De Raeve L, Langereis M, Peeraer L, Wouters J, & van Wieringen A. (2013). Expressive vocabulary, morphology, syntax and narrative skills in profoundly deaf children after early cochlear implantation. Res Dev Disabil, 34, 2008–2022. https://doi.org/10.1016/j.ridd.2013.03.003
[15] Conway CM, Karpicke J, Anaya EM, Henning SC, Kronenberger WG, & Pisoni DB. (2011). Nonverbal cognition in deaf children following cochlear implantation: motor sequencing disturbances mediate language delays. Dev Neuropsychol, 36, 237–254. https://doi.org/10.1080/87565641.2010.549869
[16] [Niparko JK, Tobey EA, Thal DJ, Eisenberg LS, Wang NY, Quittner AL, et al. (2010). Spoken language development in children following cochlear implantation. JAMA, 303, 1498–1506. https://doi.org/10.1001/jama.2010.451
[17] Kral A, Kronenberger WG, Pisoni DB, & O'Donoghue GM. (2016). Neurocognitive factors in sensory restoration of early deafness: a connectome model. Lancet Neurol, 15(6), 610–621. https://doi.org/10.1016/S1474-4422(16)00034-X
[18] Kronenberger WG, Beer J, Castellanos I, Pisoni DB, Miyamoto RT, Wilson BS, et al. (2014). Neurocognitive risk in children with cochlear implants. JAMA Otolaryngol Head Neck Surg, 140(7), 608-615. https://doi.org/10.1001/jamaoto.2014.757
[19] Council on Children with Disabilities, Section on Developmental Behavioral Pediatrics, & Bright Futures Steering Committee. (2006). Identifying infants and young children with developmental disorders in the medical home: an algorithm for developmental surveillance and screening. Pediatrics, 118(1), 405-420. https://doi.org/10.1542/peds.2006-1231
[20] Richter LM, Daelmans B, Lombardi J, Heymann J, Lopez Boo F, Britto PR, et al. (2017). Investing in the foundation of sustainable development: pathways to scale up for early childhood development. Lancet, 389(10064), 103–118. https://doi.org/10.1016/S0140-6736(16)31698-1
[21] Zhao J, Yu Z, Sun X, Wu S, Zhang J, Zhang D, et al. (2022). Association Between Screen Time Trajectory and Early Childhood Development in Children in China. JAMA Pediatr, 176(8), 768-775. https://doi.org/10.1001/jamapediatrics.2022.1630
[22] Filgueiras A, Pires P, Maisonette S, & Landeira-Fernandez J. (2013). Psychometric properties of the Brazilian-adapted version of the Ages and Stages Questionnaire in public child daycare centers. Early Hum Dev, 89(8), 561-576. https://doi.org/10.1016/j.earlhumdev.2013.02.005
[23] Govaerts PJ, De Beukelaer C, Daemers K, De Ceulaer G, Yperman M, Somers T, et al. (2002). Outcome of cochlear implantation at different ages from 0 to 6 years. Otol Neurotol, 23, 885-890. https://doi.org/10.1097/00129492-200211000-00013
[24] Archbold S, Lutman ME, & Marshall DH. (1995). Categories of auditory performance. Ann Otol Rhinol Laryngol Suppl, 166, 312–314.
[25] Doyle J. (1987). Reliability of audiologists' ratings of the intelligibility of hearing-impaired children's speech. Ear Hear, 8(3), 170-174. https://doi.org/10.1097/00003446-198706000-00007
[26] Squires J, Twombly E, Bricker D, & Potter L. (2009). Ages & Stages Questionnaires, (ASQ-3): User's Guide. Paul H. Brookes Publishing Co.
[27] Bian X, Yao G, Squires J, Hoselton R, Chen CI, Murphy K, et al. (2012). Translation and use of parent-completed developmental screening test in Shanghai. J Early Child Res, 10(2), 162-175.
[28] Heo KH, Squires J, & Yovanoff P. (2008). Cross-cultural adaptation of a pre-school screening instrument: comparison of Korean and US populations. J Intellect Disabil Res, 52(Pt 3), 195-206. https://doi.org/10.1111/j.1365-2788.2007.01000.x
[29] Saihong P. (2010). Use of screening instrument in Northeast Thai early childcare settings. Procedia Soc Behav Sci, 7, 97-105. https://doi.org/10.1016/j.sbspro.2010.10.015
[30] Tong L, Strong MK, Kaur T, Juiz JM, Oesterle EC, Hume CR, et al. (2015). Selective deletion of cochlear hair cells causes rapid age-dependent changes in the spiral ganglion and cochlear nucleus neurons. J Neurosci, 35, 7878–7891. https://doi.org/10.1523/JNEUROSCI.2179-14.2015
[31] Allen C, Nikolopoulos TP, Dyar D, & O'Donoghue GM. (2001). Reliability of a rating scale for measuring speech intelligibility after pediatric cochlear implantation. Otol Neurotol, 22, 631–633. https://doi.org/10.1097/00129492-200109000-00012
[32] Holt RF, & Kirk KI. (2005). Speech and language development in cognitively delayed children with cochlear implants. Ear Hear, 26, 132–148. https://doi.org/10.1097/00003446-200504000-00003
[33] Wie OB. (2010). Language development in children after receiving bilateral cochlear implants between 5 and 18 months. Int J Pediatr Otorhinolaryngol, 74, 1258–1266. https://doi.org/10.1016/j.ijporl.2010.07.026
[34] Beijing Mental Development Cooperative Group. (1985). Gesell Developmental Diagnosis Scale. Beijing Mental Development Cooperative Group.
[35] Bayley N. (2006). Bayley Scales of Infant and Toddler Development Administration Manual. Pearson.
[36] Frankenburg WK, & Dodds JB. (1967). The Denver developmental screening test. J Pediatr, 71(2), 181–191. https://doi.org/10.1016/s0022-3476(67)80070-2
[37] Kral A, Dorman MF, & Wilson BS. (2019). Neuronal development of hearing and language: Cochlear implants and critical periods. Annu Rev Neurosci, 42, 47–65. https://doi.org/10.1146/annurev-neuro-080317-061513
[38] Zanetti D, & Meli A. (2024). Congenital deafness and vestibular disorders: a systematic literature review. Acta Otorhinolaryngol Ital, 44(Supp. 1), S1-S12. https://doi.org/10.14639/0392-100X-suppl.1-44-2024-01
[39] Fallon JB, Irvine DR, & Shepherd RK. (2008). Cochlear implants and brain plasticity. Hear Res, 238, 110–117. https://doi.org/10.1016/j.heares.2007.08.004
[40] Wei QW, Zhang JX, Scherpbier RW, Zhao CX, Luo SS, Wang XL, et al. (2015). High prevalence of developmental delay among children under three years of age in poverty-stricken areas of China. Public Health, 129(12), 1610-1617. https://doi.org/10.1016/j.puhe.2015.07.036
[41] Falzone C, Guerzoni L, Ghiselli S, Franchomme L, Nicastri M, Mancini P, et al. (2025). Early Cochlear Implant Promotes Global Development in Children with Severe-to-Profound Hearing Loss. Audiol Res, 15(5), 121. https://doi.org/10.3390/audiolres15050121
[42] Bruijnzeel H, Ziylan F, Stegeman I, Topsakal V, & Grolman W. (2016). A systematic review to define the speech and language benefit of early (<12 months) pediatric cochlear implantation. Audiol Neurootol, 21(2), 113–126. https://doi.org/10.1159/000443363
[43] Mitchell RM, Christianson E, Ramirez R, Onchiri FM, Horn DL, Pontis L, et al. (2020). Auditory comprehension outcomes in children who receive a cochlear implant before 12 months of age. Laryngoscope, 130(3), 776–781. https://doi.org/10.1002/lary.28061
[44] Colletti L, Mandala M, Zoccante L, Shannon RV, & Colletti V. (2011). Infants versus older children fitted with cochlear implants: performance over 10 years. Int J Pediatr Otorhinolaryngol, 75, 504–509. https://doi.org/10.1016/j.ijporl.2011.01.005
[45] Elbro C, Dalby M, & Maarbjerg S. (2011). Language-learning impairments: a 30-year follow-up of language-impaired children with and without psychiatric, neurological and cognitive difficulties. Int J Lang Commun Disord, 46, 437–448. https://doi.org/10.1111/j.1460-6984.2011.00004.x
[46] Dettman SJ, Dowell RC, Choo D, Arnott W, Abrahams Y, Davis A, et al. (2016). Long-term communication outcomes for children receiving cochlear implants younger than 12 months: a multicenter study. Otol Neurotol, 37(2), e82-95. https://doi.org/10.1097/MAO.0000000000000915
[47] Wu SS, Sbeih F, Anne S, Cohen MS, Schwartz S, Liu YC, et al. (2023). Auditory Outcomes in Children Who Undergo Cochlear Implantation Before 12 Months of Age: A Systematic Review. Otolaryngol Head Neck Surg, 169, 210–220. https://doi.org/10.1002/ohn.284
[48] Laksono AD, Wulandari RD, Amaliah N, & Wisnuwardani RW. (2022). Stunting among children under two years in Indonesia: Does maternal education matter? PLoS One, 17(7), e0271509. https://doi.org/10.1371/journal.pone.0271509
[49] Murri A, Cuda D, Guerzoni L, & Fabrizi E. (2015). Narrative abilities in early implanted children. Laryngoscope, 125(7), 1685-1690. https://doi.org/10.1002/lary.25084
[50] Nagel M, & Sharman R. (2019). The Encyclopedia of Child and Adolescent Development. Wiley.
[51] Horn DL, Pisoni DB, & Miyamoto RT. (2006). Divergence of fine and gross motor skills in prelingually deaf children: implications for cochlear implantation. Laryngoscope, 116, 1500–1506. https://doi.org/10.1097/01.mlg.0000230404.84242.4c
[52] Gheysen F, Loots G, & Van Waelvelde H. (2008). Motor development of deaf children with and without cochlear implants. J Deaf Stud Deaf Educ, 13(2), 215–224. https://doi.org/10.1093/deafed/enm053
[53] Edwards LC, Frost R, & Witham F. (2006). Developmental delay and outcomes in pediatric cochlear implantation: implications for candidacy. Int J Pediatr Otorhinolaryngol, 70(9), 1593–1600. https://doi.org/10.1016/j.ijporl.2006.04.008
[54] Xiong Y, Hu X, Cao J, Shang L, Yao Y, & Niu B. (2024). Development of gross motor skills in children under the age of 3 years: a decision tree approach. Front Public Health, 12, 1421173. https://doi.org/10.3389/fpubh.2024.1421173
[55] Iverson JM, & Goldin-Meadow S. (2005). Gesture paves the way for language development. Psychol Sci, 16, 367–371. https://doi.org/10.1111/j.0956-7976.2005.01542.x
[56] Freeman V, & Pisoni DB. (2017). Speech rate, rate-matching, and intelligibility in early-implanted cochlear implant users. J Acoust Soc Am, 142(2), 1043. https://doi.org/10.1121/1.4998590
[57] Monshizadeh L, Vameghi R, Rahimi M, Sajedi F, Hashemi SB, & Yadegari F. (2021). Is there any association between language acquisition and cognitive development in cochlear-implanted children? J Int Adv Otol, 17(3), 195-199. https://doi.org/10.5152/iao.2021.8990
Type
Published
Issue
Section
License
Copyright (c) 2026 Head and Neck Diseases Conflux

This work is licensed under a Creative Commons Attribution 4.0 International License.







