A Case of Epstein-Barr Virus Encephalitis Misdiagnosed as Glioma
DOI:
https://doi.org/10.71321/c09vcg29Keywords:
Epstein-Barr Virus Encephalitis, Glioma, Brain biopsy, Tumor-like lesionsAbstract
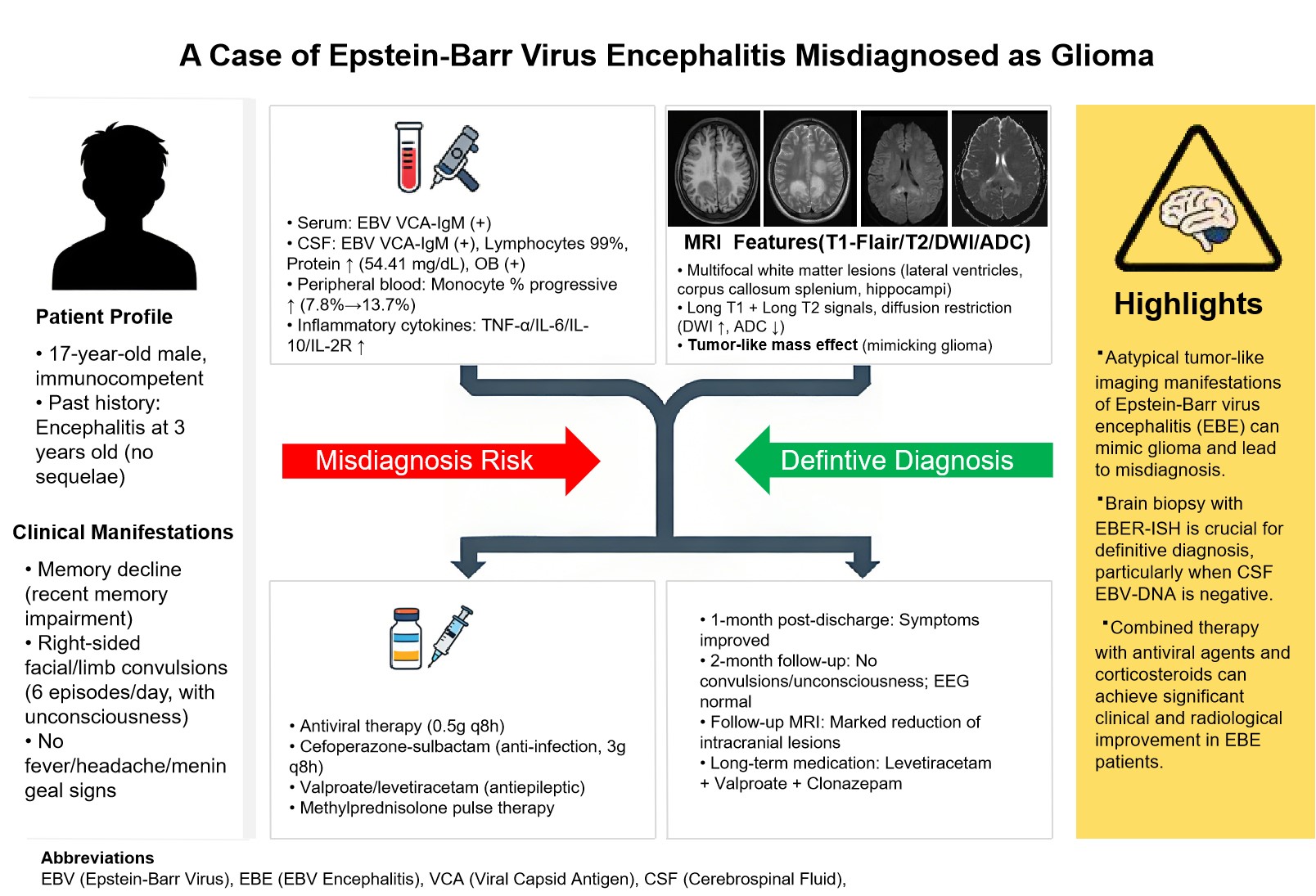
Epstein-Barr virus (EBV) infection can cause central nervous system damage, primarily manifesting as encephalitis, with diverse imaging presentations. We report a case of an EBV-infected patient who presented clinically with cognitive impairment and limb convulsions. Serum and cerebrospinal fluid tests were positive for EBV viral capsid antigen IgM. Cranial MRI revealed multifocal white matter lesions distributed along the lateral ventricles, demonstrating T1 and T2 hyperintensity with associated diffusion restriction in the involved areas, patchy enhancement, and a tumor-mimicking appearance with significant mass effect. Brain biopsy confirmed viral encephalitis. After treatment with antiviral agents and corticosteroids, the patient's symptoms improved. Follow-up cranial MRI one month later showed significant reduction of the lesions. In clinical practice, it is important to be alert to the tumor-like imaging manifestations of EBV encephalitis. Pathological biopsy of brain tissue plays a crucial role in distinguishing this condition from diseases such as glioma.
References
[1] Saeed M, Dabbagh O, Al-Muhaizae M, Dhalaan H, Chedrawi A (2014). Acute disseminated encephalomyelitis and thrombocytopenia following Epstein-Barr virus infection. J Coll Physicians Surg Pak, 24 Suppl 3:S216-218.
[2] Mazur-Melewska K, Breńska I, Jończyk-Potoczna K, Kemnitz P, Pieczonka-Ruszkowska I, Mania A, et al. (2016). Neurologic Complications Caused by Epstein-Barr Virus in Pediatric Patients. J Child Neurol, 31(6):700–8. https://doi.org/10.1177/0883073815613563.
[3] Bharucha T, Houlihan CF, Breuer J (2019). Herpesvirus Infections of the Central Nervous System. Semin Neurol, 39(03):369–82. https://doi.org/10.1055/s-0039-1687837.
[4] Liu Z, Peng A, Huang L, Sha L, Tang Y, Zhou Y, et al. (2025). Clinical features and risk factors for Epstein-Barr virus-associated encephalitis: a retrospective cohort study. Virol J, 22(1):141. https://doi.org/10.1186/s12985-025-02768-w.
[5] Louveau A, Smirnov I, Keyes TJ, Eccles JD, Rouhani SJ, Peske JD, et al. (2015). Structural and functional features of central nervous system lymphatic vessels. Nature, 523(7560):337–41. https://doi.org/10.1038/nature14432.
[6] Zhang S, Feng J, Shi Y (2016). Transient widespread cortical and splenial lesions in acute encephalitis/encephalopathy associated with primary Epstein–Barr virus infection. International Journal of Infectious Diseases, 42:7–10. https://doi.org/10.1016/j.ijid.2015.11.009.
[7] Guerrero-Ramos A, Patel M, Kadakia K, Haque T (2014). Performance of the Architect EBV Antibody Panel for Determination of Epstein-Barr Virus Infection Stage in Immunocompetent Adolescents and Young Adults with Clinical Suspicion of Infectious Mononucleosis. Clin Vaccine Immunol, 21(6):817–23. https://doi.org/10.1128/CVI.00754-13.
[8] Peuchmaur M, Voisin J, Vaillant M, Truffot A, Lupo J, Morand P, et al. (2023). Epstein-Barr Virus Encephalitis: A Review of Case Reports from the Last 25 Years. Microorganisms, 11(12):2825. https://doi.org/10.3390/microorganisms11122825.
[9] Tyler KL (2018). Acute Viral Encephalitis. N Engl J Med, 379(6):557–66. https://doi.org/10.1056/NEJMra1708714.
[10] Yanagisawa K, Tanuma J, Hagiwara S, Gatanaga H, Kikuchi Y, Oka S (2013). Epstein-Barr Viral Load in Cerebrospinal Fluid as a Diagnostic Marker of Central Nervous System Involvement of AIDS-related Lymphoma. Intern Med, 52(9):955–9. https://doi.org/10.2169/internalmedicine.52.9088.
[11] Shimizu H, Saitoh T, Koya H, Yuzuriha A, Hoshino T, Hatsumi N, et al. (2011). Discrepancy in EBV-DNA load between peripheral blood and cerebrospinal fluid in a patient with isolated CNS post-transplant lymphoproliferative disorder. Int J Hematol, 94(5):495–8. https://doi.org/10.1007/s12185-011-0951-3.
[12] Gupta RK, Soni N, Kumar S, Khandelwal N (2012). Imaging of central nervous system viral diseases. J Magn Reson Imaging, 35(3):477–91. https://doi.org/10.1002/jmri.22830.
[13] Tunkel AR, Glaser CA, Bloch KC, Sejvar JJ, Marra CM, Roos KL, et al. (2008). The Management of Encephalitis: Clinical Practice Guidelines by the Infectious Diseases Society of America. Clinical Infectious Diseases, 47(3):303–27. https://doi.org/10.1086/589747.
[14] Andersen O, Ernberg I, Hedström AK (2023). Treatment Options for Epstein-Barr Virus-Related Disorders of the Central Nervous System. IDR,Volume 16:4599–620. https://doi.org/10.2147/IDR.S375624.
Type
Published
Data Availability Statement
The clinical and imaging data supporting the findings of this case report are not publicly available in order to protect the patient's privacy and confidentiality. Anonymized data may be made available by the corresponding author upon reasonable request, subject to ethical approvals.
Issue
Section
License
Copyright (c) 2025 Brain Conflux

This work is licensed under a Creative Commons Attribution 4.0 International License.







